A 2-year-old MN Malti-poo was presented for recheck examination after being evaluated at an emergency facility for anorexia, diarrhea, and a pruritic face. Abnormalities on blood work at the emergency facility were elevated ALT activity and bilirubinuria. Physical examination was unremarkable. CBC and blood chemistry showed leukocytosis, neutrophilia, monocytosis, elevated BUN, high BUN/Creatinine ratio, and mild hypocalcemia. Urinalysis was normal. Urine culture yielded no growth.
A 2-year-old MN Malti-poo was presented for recheck examination after being evaluated at an emergency facility for anorexia, diarrhea, and a pruritic face. Abnormalities on blood work at the emergency facility were elevated ALT activity and bilirubinuria. Physical examination was unremarkable. CBC and blood chemistry showed leukocytosis, neutrophilia, monocytosis, elevated BUN, high BUN/Creatinine ratio, and mild hypocalcemia. Urinalysis was normal. Urine culture yielded no growth.
Case Study
03-00143 Cody H Microvascular dysplasia and portoazygous shunt—–RESEARCH ONLY—–
Sonographic Differential Diagnosis
Spleno azygos shunt. Slight microhepatica.
Image Interpretation
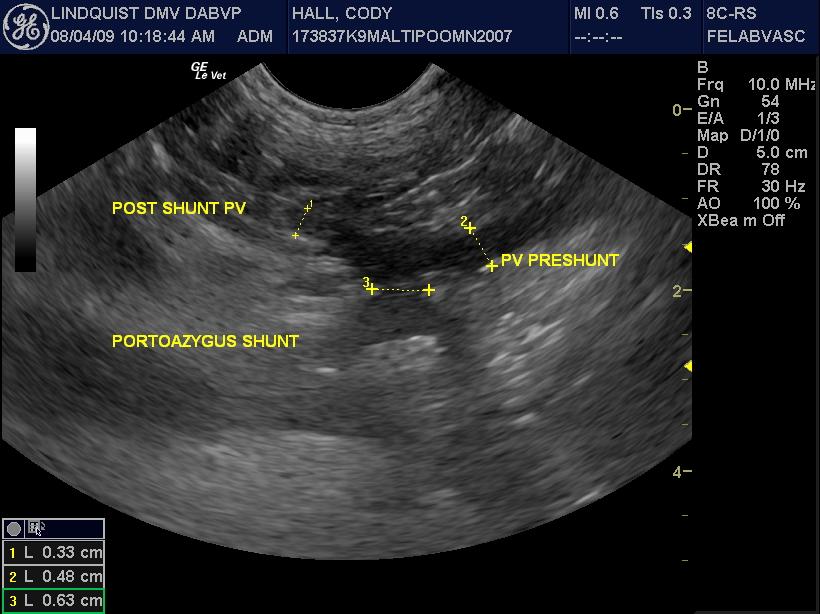
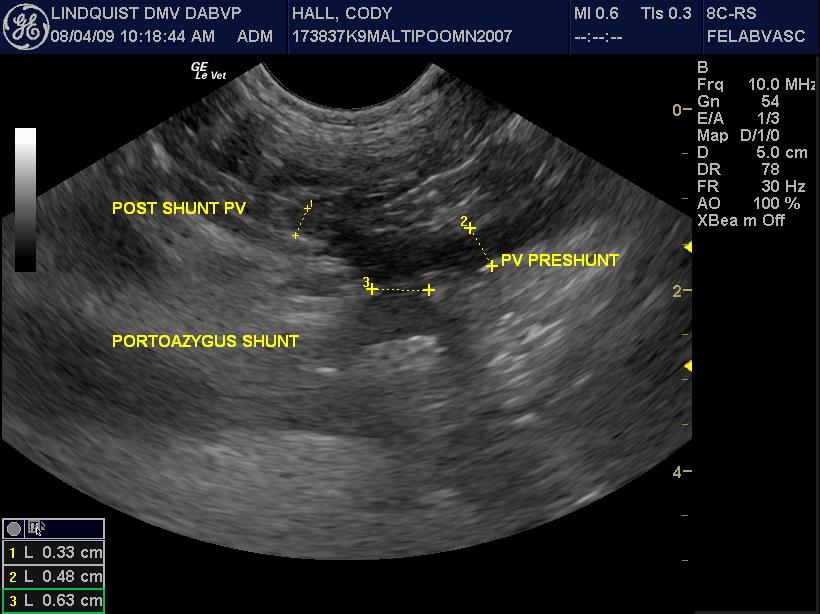
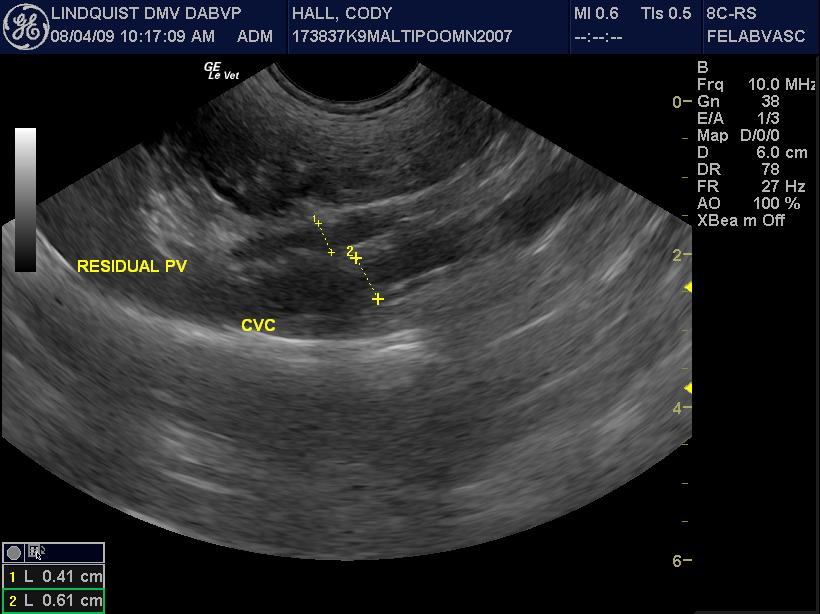
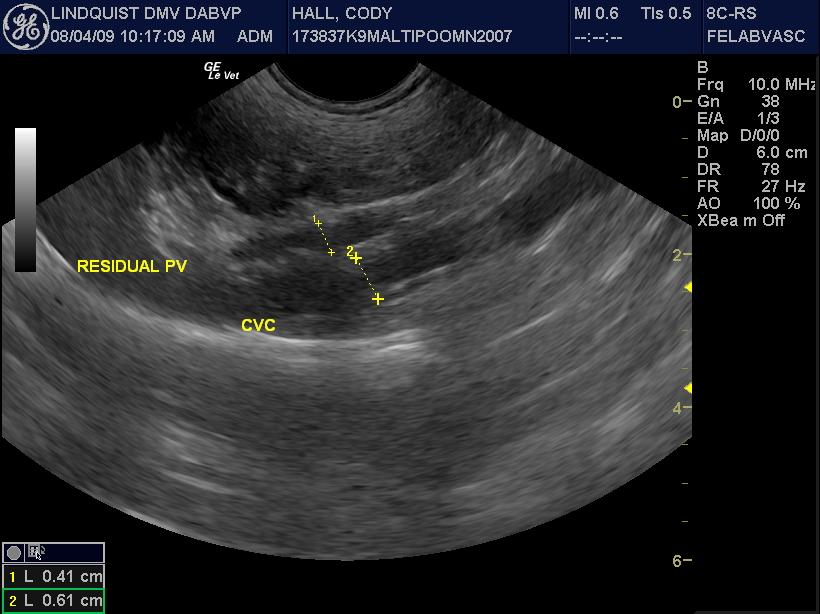
The liver was slightly subnormal in size with no significant parenchymal changes. The common bile duct was normal. The gallbladder was normal. However a 0.61cm splenoazygos shunt was noted deriving from the area of the portal vein approximately 2cm prior to the portal hilus and going dorsally and continuing into the thoracic inlet along the region of the esophagus and the aorta consistent with splenoazygos shunt. The shunt width was 0.61cm. The portal vein prior to the shunt was approximately 0.5cm and after the shunt entering into the portal hilus was 0.33cm. The portal vein to vena cava ratio was 0.4 to 0.6 respectively. The aorta to vena cava ratio was essentially 1 to 1 with the vena cava at 0.72 and 0.8 in that position.
DX
Outcome
Pre-and post-prandial bile acids were elevated (17 and 72.7, respectively). Ultrasound showed no evidence of a liver shunt. The recommendation for this patient was to continue to treat the gastroenteritis with supportive care, fluids, gastroprotectants, Metronidazole, and fed L/D diet. Repeat bile acids within 4-6 weeks and recheck ultrasound within 3-6 months were both recommended. Recheck bile acid results showed ongoing elevation – pre-prandial of 24.9 and post-prandial of 59.1. On blood chemistry elevated AST and ALT activity and hyperkalaemia was present. ACTH stimulation was within normal range. Fecal examination was negative. A portal azygous shunt was found with the follow-up ultrasound. The patient subsequently underwent portosytemic shunt ligation with ameroid constrictor placement, cystotomy, and liver biopsy; and was discharged with clavamox and K/D diet.
Comments
Outcome is confusing! Should this be broken down into more than one case due to change in diagnosis on subsequent US? Only received last US which showed shunt. Could try to get older ones. I don`t understand this sentence: "The portal vein to vena cava ratio was 0.4 to 0.6 respectively." Are those raw numbers or two ratios? I can`t tell what the video is of. Smeary. If we keep this case will need to anonymize jpgs Fern
Clinical Differential Diagnosis
Acute GI disease – infectious/dietary/toxic, liver disease – infectious/toxic/trauma/MVD
Sampling
Surgical biopsy of the liver and cystolith analysis.
Video
Patient Information
Clinical Signs
- Anorexia
- Diarrhea
- Skin Lesion
Blood Chemistry
- ALT (SGPT), High
- BUN high
- BUN/Creatinine Ratio, High
- Calcium, Low
CBC
- Monocytes, High
- Neutrophils, High
- WBC, High
Clinical Signs
- Anorexia
- Diarrhea
- Skin Lesion
Urinalysi
- Bilirubin Present
- Culture negative